By Dr. Antti Rintanen, MD, MSc
Trauma is an experience — or series of experiences — in which a real or perceived threat is encountered, often accompanied by overwhelming stress or loss of control. Most people have experienced at least one traumatic experience in their lifetime. However, only a small percentage develop an actual post-traumatic stress disorder (PTSD).
Many of my trauma patients come to my office with physical symptoms, such as chest pain, palpitations, insomnia, or loss of appetite. Often an underlying somatic cause is sought for the symptoms. Sometimes, one is found. But often, what we are seeing reflects the body “keeping the score“.
Trauma recalibrates the nervous system, preparing it for danger and threat — even when the danger no longer exists.
Healing from trauma does not mean forgetting what happened. Rather, it involves retraining the nervous system to recognise a past threat as distinct from a present, non-threatening situation.
DISCLAIMER: While I am a practising doctor, the information on this site is for educational purposes only. It does not take into account your personal circumstances, which can significantly affect medical decision-making and treatment. This content therefore does not constitute medical advice, and should not be relied upon for diagnosis or treatment. Always consult a qualified healthcare provider regarding any health concerns.
This article was written by a guest writer, and published on the 23/03/2026 using up-to-date sources at that time. Please be aware that medical information and guidelines change often.
When the nervous system changes
A traumatic stimulus/event — or prolonged hyperarousal (a state in which the nervous system remains persistently activated and on high alert) — causes an exceptionally high stress response in the body. Trauma shapes the nervous system so that it adapts to overwhelming danger or threat. If the stimulus is sufficiently intense or prolonged, some of these adaptations may persist long after the traumatic event has passed. What was once protective can become maladaptive.

Research shows that traumatic experiences lead to persistent alterations in stress response systems, creating lasting changes in how the body and brain communicate. When trauma persists, the sympathetic nervous system (SNS) — the body’s built-in fight-or-flight system — can remain switched on even when there is no immediate danger.
Biologically, this involves increased activity of stress hormones such as adrenaline and noradrenaline, which prepare the body for action. At the same time, changes in the brain’s natural anxiety-buffering mechanisms involving serotonin and gamma-aminobutyric acid (GABA) reduce the brain’s ability to settle anxiety and return to a sense of safety [1].
A dysregulated nervous system leads to increased autonomic reactivity during stressful situations. The autonomic nervous system (ANS) controls bodily functions that operate automatically — such as heart rate, breathing, blood pressure, and digestion — playing a central role in how the body responds to stress.

The ANS is made up of two main branches: the SNS, which activates the “fight or flight” response, and the parasympathetic nervous system (PNS), which supports rest, recovery, and digestion. When this system becomes dysregulated, these branches may no longer balance effectively, resulting in excessive arousal or difficulty returning to a calm state.
A meta-analysis of youths with post-traumatic stress symptoms found small but significant associations between symptoms and heightened autonomic activity during stress tasks, with some evidence of increased sympathetic activity at rest[2]. Understanding these changes at a physiological level can help inform prevention and treatment of PTSD.
A dysregulated nervous system loses its flexibility. It is no longer able to smoothly switch between activation and rest states. Instead, it becomes survival-oriented, prioritising threat recognition over recovery and rest.
The body remembers
Trauma is not just psychological — it causes whole-body responses that are measurable. Some of my trauma patients show significantly elevated markers of SNS activation such as decreased heart rate variability, along with symptoms such as chest pain, palpitations, insomnia, and loss of appetite. People may also experience digestive disturbances, changes in immune function, increased inflammation, headaches, or chronic fatigue.
For trauma patients, the hypothalamic-pituitary-adrenal (HPA) axis, which plays a central role in coordinating stress responses, often shows sustained dysregulation. Chronic dysregulation of these systems can lead to functional impairment in individuals who become “psychologically traumatised” [1]. For example, the prefrontal cortex, which normally modulates emotional responses thus playing a role in the HPA axis, shows decreased activation [1]. As a result, this sensitised system detects dangers and threats very acutely but is unable to down-regulate effectively when the threat has gone. In daily life, this may appear as difficulty recovering from stress, persistent fatigue, increased sensitivity to pain, sleep disturbance, emotional reactivity, or problems with concentration and decision-making.
Our somatosensory system, which is responsible for perceiving our physical bodily sensations, is very sensitive to disruption [3]. When trauma occurs, this system, which normally integrates sensation and maintains bodily safety, becomes dysregulated. When this occurs, sometimes even normal sensations can trigger the stress system and the body feels unsafe even when there is no actual threat.
Why gentle movement matters
Body-and movement-oriented interventions (BMOI) have received more attention over the last couple of decades. BMOI are not just about relaxation, but directly influence nervous systems that have been disrupted by trauma. BMOI are “bottom-up” strategies, while cognitive methods are “top-down” strategies.
Top-down strategies — such as talking therapy, cognitive behavioural therapy, or mindfulness meditation — work through thinking, reflection, and conscious emotional processing. They help the brain interpret situations, regulate emotions, and change behavioural responses. Bottom-up strategies — such as yoga, tai chi, sensorimotor psychotherapy, or body-based mindfulness exercises — work through the body and nervous system directly, helping the brain and body relearn safety, regulate stress responses, and release physical tension. Both approaches are complementary and often most effective when used together.

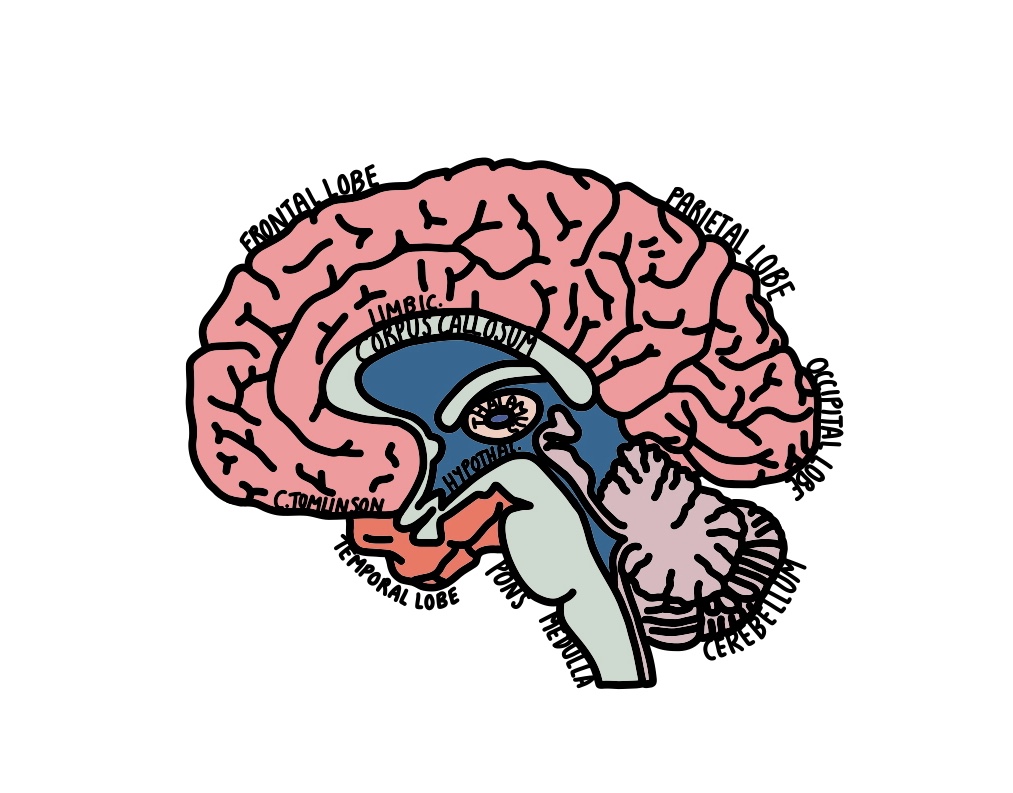
Bottom-up strategies directly activate subcortical* structures such as the limbic system and the brainstem, via different pathways than top-down cognitive methods. These subcortical structures are evolutionarily older, and bottom-up strategies may activate them more deeply than top-down strategies can [4].
There are several movement and body-based methods. Movement-based interventions include trauma-sensitive yoga, tai chi and qigong, as well as slow walking or gentle stretching performed at a steady, predictable pace, allowing the nervous system to experience movement without triggering alarm responses.
These are complemented by body-oriented psychotherapeutic approaches, such as sensorimotor psychotherapy, which integrates body awareness with traditional psychotherapy; somatic experiencing, which focuses on gradually releasing stored survival responses in the nervous system; and body-based trauma therapy, which uses posture, movement, and sensation awareness as part of psychological healing. In addition, there are methods that focus on breathing and body awareness, such as mindfulness-based stretching and postural awareness exercises.
A systematic review and meta-analysis of BMOI interventions for PTSD found a medium effect size for symptom reduction, with results sustained at follow-up [4]. Across 15 studies — including various forms of yoga, sensorimotor psychotherapy, and other body-based approaches — participants showed significant improvements not only in PTSD symptoms but also in comorbid depression.
Yoga, specifically, has demonstrated significant benefits across multiple studies. A meta-analysis of 20 randomised controlled trials (RCTs) — studies that compare an intervention with another treatment or standard care under controlled conditions — found that yoga significantly improved self-reported PTSD symptoms and both immediate and long-term depression symptoms [5]. The effects remained stable or improved at follow-up assessments, suggesting lasting benefits rather than temporary relief.

In one RCT with women diagnosed with chronic, treatment-resistant PTSD, 10 weeks of trauma-sensitive yoga significantly reduced PTSD symptoms compared to participants who received general women’s health education and supportive discussion sessions rather than movement-based therapy, with effects comparable to established psychotherapeutic approaches [6]. Many participants showed clinically meaningful reductions in PTSD symptoms following the intervention. Another RCT in healthcare workers with trauma-related symptoms found that mindfulness-based stretching and deep breathing reduced PTSD symptoms significantly [7].
Thus, bottom-up interventions can reach different or deeper levels than cognitive therapy alone. The most effective combination, however, is a combination of both. BMOI methods are especially useful for patients in whom cognitive therapies have not produced sufficient recovery. The effectiveness of BMOI methods supports our understanding that trauma involves dysregulation of the nervous system, rather than existing solely as a psychological memory or personal narrative.
*Subcortical refers to deeper brain structures beneath the outer thinking layer of the brain (the cortex), including areas involved in emotion, memory, and automatic survival responses.
Conclusion and the path forward
When assessing trauma, a more holistic biological perspective should be taken into account, in addition to the traditional top-down psychological approach. Trauma affects the nervous system at levels that cognitive top-down work alone cannot always reach. Treatment plans should also consider bottom-up body and movement-based interventions, which may reach deeper subcortical limbic systems and the brainstem.
Treatment plans should be designed to include more BMOI, especially if the patient is hyperaroused (easily startled, tense, or anxious) or hypoaroused (numb, disconnected, or sluggish), or if they experience significant physical symptoms. These interventions include movement-based interventions, body-oriented psychotherapeutic approaches, as well as breathing and body awareness exercises.
Interventions should be tailored to the patient’s situation and selected individually. Treatment modalities should be implemented gradually and emphasise patient agency. Body-based methods should be integrated into a holistic treatment plan, combining them with top-down cognitive and psychotherapeutic methods, rather than replacing them or acting as an alternative treatment.
It is also important to monitor the response to treatment. Things to monitor include symptoms, motor control, recovery ability and development of body awareness. However, it is good to remember that the patient should be referred to a professional multidisciplinary team for treatment without delay if independent practice does not bring the desired benefit or if the symptoms worsen.
Editor’s note: Reflection on this article
In this article, Dr. Antti Rintanen offers a compelling exploration of trauma as a whole-body experience, showing how dysregulation of the nervous system can affect us both physically, with symptoms we may notice, and physiologically.
His insights are strengthened by his rare dual perspective as both a medical doctor and a former elite athlete, giving him unique authority on how the body responds to stress, trauma, and healing. There is much to take away from his perspective.
Ultimately, this article encourages us to approach trauma treatment holistically, highlighting the importance of movement alongside psychological and cognitive strategies in promoting resilience, recovery, and well-being.

Dr. Antti Rintanen is a licensed medical doctor and former world champion in Taekwon-Do, with a strong interest in translating medical knowledge into clear, practical guidance for everyday life. He writes regularly at drantti.com and yogatribune.com about a broad range of health and psychosocial topics, including stress management, yoga, sleep, and recovery, as well as applied medical subjects such as athlete blood tests and supportive tools for back pain.

References
- https://pmc.ncbi.nlm.nih.gov/articles/PMC3182008/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC8858870/
- https://doi.org/10.3389/fnins.2022.1015749
- https://doi.org/10.1002/jts.22465
- https://doi.org/10.1016/j.psychres.2024.116098
- https://doi.org/10.4088/JCP.13m08561
- https://doi.org/10.1210/jc.2012-3742
AI was used during the research and drafting process.

Leave a comment